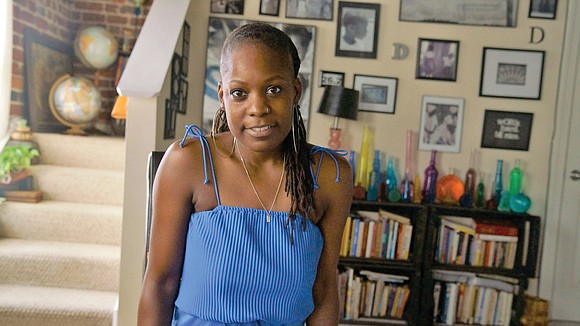Personality: Darlene A. Scott
Spotlight on Women Heart Champion and volunteer health advocate
11/15/2018, 6 a.m.
Darlene Anita Scott, an associate professor of composition and creative writing at Virginia Union University, is a long-distance runner and the image of great health and fitness.
That was two years ago.
At 41, Ms. Scott was training for her seventh marathon when she noticed that her conditioning wasn’t improving. She visited her doctor, and subsequent testing revealed she had an enlarged heart and several others issues.
“According to my doctors, I am highly functional because when I went in to see her on the day of testing, my heart was functioning at (only) 20 percent. This was after running 10 miles that morning” Ms. Scott recalls. “Most people can’t walk upstairs at that functioning rate, much less run.”
Within a year, Ms. Scott had a pacemaker implanted. An ICD, an implantable cardioverter defibrillator, was installed in June 2017. The small, electronic device is connected to the heart and is used to continuously monitor and help control fast and sometimes life-threatening electrical problems with the heart. The ICD is about the size of a stopwatch.
“Once that was in place, my physician did continuing testing to see where the enlarged heart came from,” she says. “We found out it was an autoimmune disease producing cells that fight off what they think is a threat to the body but attacks the heart, causing electrical and rhythm problems, as well as damaging tissue and causing parts of the heart to malfunction.”
Through research, she found WomenHeart: The National Coalition for Women with Heart Disease, a national nonprofit started in 1999 that helps educate and advocate for women with heart disease. The organization has 110 patient support groups in 40 states.
After working with an advocate, Ms. Scott says she wanted to help others as a WomenHeart Champion.
“That would also help me because it would give me a reason for going through the heart situation,” Ms. Scott says.” Otherwise, when I had that loneliness ‘why me?’ moment, I could be helpful to someone else. It is a learning experience for me. I also wanted to add purpose to the experience.”
Ms. Scott joined nearly 50 women in the Class of 2018 for training at the Science and Leadership Symposium at the Mayo Clinic in Rochester, Minn. The four-day symposium, led by renowned cardiologists and experts in health policy, advocacy and communications, has given Ms. Scott a foundation from which she can support other women facing or at risk for heart disease.
She is now part of a network of 850 volunteers across the country ready to help educate and advocate for women.
“We learn how to talk about heart disease in the community, as well as some of burdens people are coming with as they come seek you out as an educator,” Ms. Scott explains.
She learned about various types of heart disease, including conditions like hers, in which “there was nothing I could have done to prevent it.”
In such cases, she says, “we don’t need to talk about prevention. We need to talk about how to live with” heart disease.
She said her family, including her twin sister, has been supportive. Her twin, she said, doesn’t have an enlarged heart or heart disease.
“Trying to tell my entire family what I need is difficult because I don’t always know what I need,” she says. “But this is not their issue. I have to figure out what I need and what I am looking for in terms of support and then figure out how to ask for it,” she says.
“In the end, we are a work in progress.”
Meet this week’s heart advocate and Free Press Personality, Darlene Anita Scott:
Occupation: Professor of composition and creative writing at Virginia Union University.
No. 1 volunteer position: WomenHeart Champion with the National Coalition for Women with Heart Disease.
Date and place of birth: Feb. 1 in Milford, Del.
Current residence: Richmond’s Church Hill.
Education: Bachelor’s in English, Spelman College; and master’s in creative writing, Virginia Commonwealth University.
Family: Three older sisters, Denise, Dianne and Debra; twin sister, Doreen; parents; and eight nieces and nephews.
Why I decided to become a WomenHeart Champion: I wanted to be the person I needed (even though I didn’t always know I needed her) as I managed the punch-in-the-gut that was my heart failure diagnosis and to make meaning of what was — what is —happening to me.
My WomenHeart Champion responsibilities include: Providing education to my community about women’s risk factors, prevention and/or heart disease management by sharing information at health fairs, churches, community programs and the like. I also advocate for better research and care for women with heart disease or at risk for heart disease.
Foremost mission: To improve outcomes for women living with or at risk for heart disease by empowering, educating and advocating for them.
Heart disease is: The No. 1 killer of men and women in this country, ahead of many diseases and conditions that we talk about way more often. It’s often preventable, although not in my case or in the case of congenital or idiopathic heart conditions. And in almost all cases, whether congenital, idiopathic, or otherwise, heart disease is manageable with appropriate and timely intervention.
Why related risk factors often are missed in women: Research around heart disease largely excludes women. Most studies include more men than women. So women’s symptoms are not recognized by health care providers who have been taught what heart disease looks like in men but not in women. Women do not recognize or address their own risk factors because they are often caregivers and not receivers of care. In fact, studies show that women are more likely to seek care for someone in apparent heart distress than to seek care for themselves if they are experiencing the same.
Heart disease risk factors for women are: Lifestyle related like chronic stress, smoking and poor diet. Factors that are unique to women but are hardly known or discussed are pregnancy and menopause. It’s not clear if there’s a correlation between heart disease and the hormonal changes that take place in a woman’s life at those times. This is another reason why more studies must include and even center around women for better understanding of their experiences and thus result in better outcomes.
What women can do to reduce their risk: Practice mindful eating habits. It’s important to choose carefully what you put on your plate, like fresh fruit and vegetables. But why you’re putting it on your plate is as consequential. Eating is often social and emotional; we eat to fellowship, as reward or treat and in a rush. These habits can lead to us eating more unhealthy foods. Treats or indulgent meals have their place, but in the words of St. Augustine, “Virtue lies in moderation.” Women should also aim for 30 minutes of dedicated physical activity at least five times a week — a brisk walk, dancing, skating. And get some sleep! Adding an hour of sleep can be done in increments of 10 minutes per night over the course of a week. The cumulative effects are critical. Over time, lack of sleep can make our bodies susceptible to disease because sleep is when they rest and repair themselves. And maintaining a healthy weight can reduce your risk for, or help you manage, heart disease.
What motivated me to get involved in community service: I wanted to give purpose to my experience. I didn’t want it to be “all about me.”
How I start the day: Reminding myself to be grateful for the space between my “no longer” and “not yet.” I’ve been blessed to be “high functioning” in my condition but I’m hyper-aware of physical and mental changes, remain in the flux of treatment and have to remind myself of, and to give thanks for, my privilege(s) despite those circumstances.
A perfect day for me: Starts with a run and a resistance workout. Then I spend the day creating something in my studio, probably a collage or working on some writing. It ends with a conversation with my twin or my mom before I fall asleep with a good book.
Something I love to do that most people would never imagine: Swim. I have severe water anxiety even after taking swimming lessons over the years. There is so much peace underwater. But my body remembers an episode in which I nearly drowned, so it refuses to stay underwater without panicking.
How I unwind: Sketch or take a walk in nature.
A quote that I am inspired by: I’m a poet so I get a lot of inspiration from poetry. Lately Derek Walcott’s “Love After Love” reminds me, “You will love again the stranger who was yourself” because my condition has sometimes made me feel like a stranger in my body. And from Audre Lorde’s “For Each of You:” “When you are hungry/learn to eat/whatever sustains you/until morning/but do not be misled by details/simply because you live them.”
Best late-night snack: Homemade popcorn or roasted plantain chips.
Best thing my parents ever taught me: “Save some for yourself.”
Person who influenced me the most: My Aunt Sarah was determined (maybe a little stubborn!), fun, wise, smart, spiritual and kind. And she was my cheerleader from my most awkward uncertain adolescent days. I aspire to be that kind of model to my nieces, nephews and students.
The book that influenced me the most: “The Fall of Freddy the Leaf” by Leo Buscaglia. It’s a meditation on the cycle of life.
What I’m reading now: “Mama Day” by Gloria Naylor and “The Body Keeps the Score” by Bessel van der Kolk.
The one thing that I’ve learned in life is: Fools rush in where angels fear to tread.
My next goal: Return to distance running and complete a marathon.